In the UK, it is not currently mandatory for hospitals to collect data on surgical site infections (SSIs) following caesarean section (CS) surgery. Therefore, it is difficult to ascertain the actual rates of SSIs in women who have had a CS.
The rates of CS SSIs reported in the literature range from 3% to 18% (Errity et al, 2023; Ward et al, 2008; Wloch et al, 2012; Saeedet al, 2017).
A prospective multicentre study by Ward et al (2008) collected data from the records of 5,563 women who had undergone CS surgery in 11 UK maternity units in the East Midlands over a 2-year period. The authors found 758 (13.6%) of the women had wound problems; of these, 370 (48%) had CS incisional infections and 118 (15%) had uterine infections. Details of the other wound problems were not stated. Interestingly, 84% of these problems developed after discharge. The median hospital stay in this study was 3 days.
A study by Sangwan and Malhotra (2019) looking at the risk factors for SSI development in CS wounds found that SSIs manifested between 4 and 10 days post-operatively. The average length of hospital stay for women undergoing a CS in the UK is 3–4 days, inferring that if a woman develops an SSI post CS this would most likely be out of hospital (NHS Digital, 2024).
Regardless of what the wound problem was in the Ward et al (2008) study, it was treated with antibiotics in 99% of patients. This practice of antibiotics for any CS wound problem continues. This would seem to be contrary to recommendations for the judicious use of antibiotics, advocated for antimicrobial stewardship, when the global aim is to prevent antimicrobial resistance (World Health Organization, 2023).
More recently, Magro (2023) reported local CS SSI rates in one UK hospital as 18-32%. While it is possible that this increase compared to Ward et al (2008) could be potentially due to better reporting, the author highlighted the increase in obese pregnant women, from 22% in 2010 to 44% in 2018 (Magro, 2023).
In addition, a recent State of the Nation report carried out by the National Maternity and Perinatal Audit (NMPA, 2025) found caesarean birth rates increased considerably between 2018/19 and 2023. Unplanned caesarean birth from rose from 15.5% to 23.1% and planned caesarean births from 12.1% to 16.4% (NMPA, 2025).
A CS SSI has physical and emotional effects on the mother and is a financial and resource burden on the healthcare system (Zuarez-Easton et al, 2017; Erritty et al, 2022; Magro, 2023). In addition, there may also be an increased financial burden on the mother and extended family.
An accepted way of reducing SSIs is the use of SSI prevention bundles of care (Pellegrini et al, 2017; National Institute for Health and Care Excellence [NICE], 2020; Kuznicki et al, 2020). These bundles include pre-, peri- and post-operative aspects of care. A prospective cohort study demonstrated a cumulative reduction in SSIs in patients undergoing CS surgery as the elements of the bundle were incrementally introduced (Erritty et al, 2022).
One important element of an SSI prevention bundle is how the incision is to be dressed and for how long it will stay covered. However, anecdotally, this element appears to be actioned in maternity practice with differing post-operative dressings being employed over varied timespans of 6–72 hours for CS incisions.
In the guideline on prevention and management of surgical site infections, NICE advocates the use of an ‘interactive’ wound dressing (NICE, 2020). The caesarean birth NICE guidance suggests “removing standard dressings 6 to 24 hours after the caesarean birth” (NICE, 2025). Both these guidelines seem to create the potential for varied interpretation of recommended post-operative wound care in CS wound management.
The NICE (2025) recommendation for early removal of post-operative dressings following CS surgery is based on one small randomised controlled trial (n=320) examining 6-hour versus 24-hour dressing removal and wound complications in low-risk women who had CS surgery with no complications (Peleg et al, 2016). Indeed, the guideline does acknowledge that there was limited evidence for the recommendation (NICE, 2025).
Peleg et al (2016) defined wound complications as infection, disruption (skin dehiscence or deeper) or seroma/haematoma. The wounds were assessed for complications at discharge after a median hospital stay of 4 days (range 3–12 days) and at days 5–7 for staple removal in clinic, with no long-term follow-up. The rates of wound complications were similar in both groups – 12.5% in the 24-hour group and 13.8% in the 6-hour group.
In our opinion, the NICE guidance to remove dressings 6-24 hours after birth should be re-evaluated in view of the increase in CS wounds and the increase in obese pregnant women.
Current local practice
A local acute Trust does not have definitive guidelines on how long a post-operative dressing should remain in place following CS surgery. However, if a CS wound is thought to be deteriorating there is early referral to the tissue viability nurse (TVN) team and a wound assessment is carried out, resulting in an appropriate dressing/management regimen. There is a regional wound care formulary, and this is used when providing a wound care plan for the patient, which facilitates the smooth transition into community care using the same dressing/management regimen. Anecdotally, the midwives in this Trust report that they do not feel confident with wound management and dressing selection. It is evident from these conversations with the midwifery team that they would like support and guidance to increase their knowledge in wound care. The Trust recognises that there is a need for the introduction of a pathway for post-operative CS wound care to further support midwives.
These feelings are also common in student midwives. A short preliminary survey (local student midwife survey) conducted at a university in the East of England revealed that student midwives are exposed to varying practices and guidance depending on their placement location. Sixteen students responded to the survey, comprising nine final-year, three second-year, and four first-year students, all at the end of their academic year. Placements were undertaken in Cambridgeshire, Essex and Northwest Anglia, where notable differences in wound care management were observed.
Only 29% (n=5/16) of respondents were aware of a formalised guideline or protocol within their Trust that informed midwives’ approach to wound care. When asked which guidance was being followed, students commonly cited NICE guidelines, which is interesting as NICE (2025) does not address wound management in detail. This highlights the need for further investigation into the sources of guidance currently shaping midwifery practice.
One clear theme which emerged from the student feedback was that women were being advised by student midwives to expose their wounds to air in order to promote healing. Given that student midwives often replicate the practices they observe from qualified midwives, it can be reasonably assumed that this advice is being promoted by midwives themselves to women recovering from caesarean sections. This is despite evidence to support keeping surgical wounds covered for a minimum of 48 hours and up to 4 days (Black et al, 2020; Stryja et al, 2020). This observation was particularly noted by second and final-year students. Two respondents described the wound care advice provided by midwives as ‘vague’ or indicative of limited knowledge. Additionally, 37.5% (n=6/16) reported that women received only verbal instructions upon discharge, although 62.5% (n=10/16) were aware of signposting to digital, written and verbal resources following surgical procedures.
The most significant challenge identified by students was managing wound care for women with a raised BMI. Many felt that university education lacked sufficient content on caring for CS wounds in this population. Students also noted confusion within community settings, where guidelines are often outdated and midwives uncertain about when dressings should be removed. One student specifically highlighted the lack of clarity in documentation practices, stating that women were given vague advice and student midwives minimal guidance on what should be recorded in postnatal notes.
A key limitation of this preliminary survey is the small sample size, which restricts the generalisability of the findings. Consequently, further research is urgently needed to explore current approaches to wound care management, in the speciality of maternity, within both university education and placement settings. A larger-scale survey encompassing a broader geographic region would provide more robust insights and help inform consistent, evidence-based practice across midwifery training and clinical environments.
SSI prevention in CS surgery
Within one local acute care trust, women readmitted with SSI infections in CS wounds are seen, if requested, by the inpatient TVN team. It is important to note that surveillance of SSIs in CS wounds is not currently mandated in England, so data on numbers of women readmitted with an SSI in their CS wound is not presently collected within this acute trust. Therefore, it is presumed that a significant number of women with a CS wound problem will be managed within the community. If women are readmitted with a CS SSI, the organisation endeavours to place them on the maternity unit rather than a generic adult ward. This enables the mother to bring her newborn into hospital with her. This aims to minimise disruption to the baby’s care, feeding and bonding. In this local acute trust there is currently a proposal to introduce an SSI prevention pathway for women undergoing CS surgery.
Accordingly, it would seem to be important that women undergoing a CS follow an SSI prevention care bundle, with significant attention given to the post-operative wound care/dressing regimen. Using a SSI prevention care bundle has been demonstrated to reduce SSI rates in women who have undergone CS surgery (Pellegrini et al, 2017; Kuznicki et al, 2020; Errity et al, 2022). One important aspect of an SSI prevention care bundle is the post-operative management of the surgical site wound. As discussed above, the variability in CS wound care of which post-operative dressing to use and for how long to leave in place, appears significant.
Recent research has looked at the effectiveness of different types of wound dressings (Stanirowski et al, 2016a, 2016b; Magro, 2023) and therapies, such as prophylactic incisional negative pressure wound therapy (iNPWT) in CS wounds (Hyldig et al, 2018; Erritty et al, 2022).
In the last 10 years, dialkylcarbamoyl chloride (DACC)- coated wound dressings have come to the attention of maternity and other surgical specialities, such as vascular (Stanirowski et al, 2016b; Bua et al, 2017; Totty et al, 2019). This technology comes in a post-operative dressing, Leukomed Sorbact surgical dressing (Essity).
DACC is a fatty acid derivative that is highly hydrophobic (Cooper and Jenkins, 2016). This hydrophobicity attracts microorganisms that have hydrophobic extracellular surfaces, e.g. Staphylococcus aureus and Pseudomonas aeruginosa, locking them within the dressing, which reduces bioburden in the wound (Rippon et al, 2021). DACC-coated dressings have the potential to reduce the use of antibiotics (Husmark et al, 2022).
The effectiveness of DACC-coated wound dressings in reducing SSIs was demonstrated in a systematic review and meta-analysis by Rippon et al (2025), where they report from five studies (n=5,840) that the odds of an SSI was almost halved in patients treated with a DACC-coated dressing. Of note, three of the included studies looked at CS wounds (Stanirowski et al, 2016a, 2016b; Magro, 2023). In addition, NICE (2021) recommends the use of Leukomed Sorbact for preventing SSIs.
Taylor et al (2020) introduced a multifaceted approach to improve quality and reduce CS SSIs in one maternity service in the UK. This initiative included the introduction of Leukomed Sorbact as the post-operative dressing of choice, initially only for women with a BMI >30, moving to all women within the first year of using the dressing. This initiative saw SSI rates in CS wounds fall over a 2-year period. Of note was the change to the timing of the removal of post-operative dressings, changing from removal at 24 hours to leaving the dressing in place for up to 5 days.
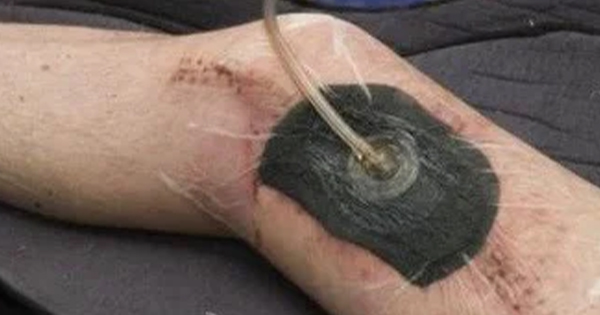
The use of iNPWT for prophylactic incisional management for surgical wounds healing by primary intention has increased over the last decade. A Cochrane systematic review concluded that iNPWT when compared to standard wound dressings probably reduces the rate of SSIs, and that further studies in specific surgeries are required (Norman et al, 2020).
Research on iNPWT in CS wounds has demonstrated varying outcomes. A randomised controlled trial of 154 women assigned to either iNPWT or standard dressing following CS surgery found no difference in wound complications between the two groups (Gonzalez et al, 2023). However, a systematic review and meta-analysis by Gu et al (2021) found a significant reduction in SSI rates in obese women after CS surgery. Erritty et al (2023) demonstrated a fall in SSI rates when iNPWT was integrated into their SSI prevention care bundle in CS surgery, along with three other interventions (skin preparation, warming blankets and vaginal cleansing). It is apparent that the use of iNPWT in CS wound care has a place within an SSI prevention bundle, but there is a need for further research into risk stratification, which would include women with a high BMI, who would most benefit from iNPWT.
Wound care education for midwives and student midwives
Midwifery educators hold a critical responsibility to design and deliver evidence-based knowledge and clinical skills to student midwives in training. The journey to becoming a qualified midwife in the UK is rigorous, encompassing a broad and complex curriculum. All approved midwifery programmes are required to ensure that, at the point of registration, students meet the competencies outlined in the Nursing and Midwifery Council (NMC) Standards of Proficiency for Midwives (NMC, 2019). These standards provide a framework for safe, effective, and person-centred care.
However, a significant challenge arises in the delivery of wound care education, specifically, the management of surgical wounds following CS surgery, due to its omission from the standards. In 2023/24, the NHS maternity statistics reported that approximately 42% of births were by CS (NHS Digital, 2024), an increase from 27.6% in 2018-19. Therefore, it would seem that wound care management should be a priority in midwifery training.
Although domains such as Safe and Effective Midwifery Care and Additional Care for Women and Newborn Infants with Complications imply the need for post-operative support, they do not include direct guidance on surgical wound management (NMC, 2019). This is a critical gap in the current curriculum and may contribute to a fragmented approach across universities and clinical placement areas. Without explicit national benchmarks, the teaching and assessment of CS wound care is left to local interpretation, resulting in variable educational experiences for student midwives nationally.
Moreover, there is a paucity of contemporary literature exploring midwives’ confidence in managing CS wounds. However, a survey by Baxter and Lymn (2015) identified that midwives (n=44) perceived a need for further education in this area and reported low confidence in delivering post-operative wound care.
Given that midwives are the principal providers of postnatal care, it is imperative that wound management is delivered in an evidence-based and consistent manner to ensure optimal maternal outcomes. If qualified midwives lack confidence in CS wound care, as that study suggests, this may adversely affect their ability to mentor and educate student midwives, perpetuating the cycle of under-preparedness.
To address this educational deficit, several recommendations can be proposed. These include increasing clinical placements in post-surgical recovery settings, integrating lectures delivered by subject-matter experts, such as TVNs and experienced midwives, and embedding structured wound care modules within the curriculum.
Furthermore, national curriculum reform should prioritise the inclusion of surgical wound care competencies, supported by clear learning outcomes and assessment criteria. This is supported by Taylor et al (2020), who, in their quality improvement package in reducing CS wound SSIs, advocate that wound care is part of mandatory training, and that midwives and support workers in maternity units must have access to this training. Additional research is needed to evaluate current teaching practices across universities and placement sites, and to explore midwives’ preparedness and confidence in this domain.
Further Recommendations
The UK Health Security Agency (2025) strongly encourages participation in its Surgical Site Infection Surveillance Service for CS surgery. However, it is not mandated to collect SSI rates in CS surgery in England. This paper would recommend that maternity services explore introducing SSI surveillance for a minimum of one quarter per year. This would go some way towards developing a real picture of how many women undergoing CS surgery develop an SSI, which in turn would assist in having standardised wound care management regimens.
Both the use of DACC-coated dressing and iNPWT in CS wound care should be considered for wound management post CS surgery. iNPWT, alongside risk stratification for its use, should be available to women with a high BMI and/or have had repeated CS surgery. Educational deficits in the area need to be addressed by embedding structured wound care modules within the curriculum of student midwives with ongoing post registration local education packages for both student and qualified midwives.
In our opinion, the NICE guidance to remove dressings 6-24 hours after birth should be re-evaluated in view of the increase in CS wounds and the increase in obese pregnant women.
Conclusion
This paper has highlighted that there is differing advice on the management of CS wounds in practice and that there is currently a need for discussion and consensus on the management of CS wounds. This needs to be accompanied by specific CS wound care education for both student and qualified midwives.