In 2019 Knowledge For Change (K4C), together with the University of Salford, Kabarole Health District, Fort Portal Regional Referral Hospital (FPRRH) and the Pharmaceutical Society of Uganda established the importance of wound care to reduce maternal mortality from sepsis and the effective antimicrobial stewardship in Uganda (Ackers, et al, 2020). From this work it was identified that nurses and midwives had to be at the heart of any multidisciplinary approach to future care delivery.
Capitalising on the impact of ‘knowledge clusters’ (UK professionals working alongside K4C and local health workers) and the use of virtual international experiences in undergraduate programmes (Stephens and Hennefer, 2013), three midwives from Uganda were supported in applying for Commonwealth Fellowships to Salford in 2021. Their fellowships would be used for knowledge and skill development in wound and acute illness management; and on return the Commonwealth Fellows would lead the development and delivery of six virtual wound care clinics from September to December 2021. The purpose of the virtual clinics was to influence current practice in FPRRH enabling the midwives to conduct a review of wound management processes, examine the current evidence base and use the case studies from the clinics to develop guidance based on the resources and services available. The clinics would also provide students studying on the Tissue Viability Module at the University of Salford an opportunity to experience wound management in both a global and interprofessional context, as the cases presented at the clinics exposed them to varying patient populations which were discussed by members of the interprofessional team. The experience could be considered to be similar to that of an international elective for a pre-registration student (Addis et al, 2022).
There were six virtual wound clinics developed and delivered by the Fellows and clinicians in FPRRH between September 2021 and December 2021. Preparation of these were guided by academic colleagues at the University of Salford. An interprofessional team at FPRRH comprising of nurses, midwives, pharmacists, doctors, clinical officers, and healthcare volunteers joined with lecturers on the Tissue Viability module, and their students, in a virtual bi-weekly forum.
The format of the virtual clinics was refined following two early pilot ‘live-stream’ clinics during the Fellows’ time in Salford (March –July 2021), which identified ethical and logistical issues relating to showing the live ward environment and to enable more FPRRH staff to join without disrupting clinical work.
At each clinic a case (adult or child with a wound) was presented by the Fellows and FPRRH team. Wound and care management was discussed in depth and across professions and countries, for example wound assessment and aetiology, wound bioburden, surgical techniques, dressing choice and purchase, pharmacology, biochemistry, IV fluids, nutrition, and emotional care.
In order for the University of Salford students to have an awareness of the economic, social and environmental factors affecting healthcare and wound management in Uganda, background information regarding the hospital and its services were shared on the module virtual learning platform. The students were directed to this information during the clinics when considering their clinical reasoning and decision-making processes. FPRRH is a public internship hospital in the town of Kabarole District, Western Uganda. The Ugandan Ministry of Health fund general care in the hospital. Services within the hospital include maternity, paediatrics, burns, high dependency, medicine and surgery. Wound care products available include normal saline, water, hydrogen peroxide, savlon, iodine, honey, sugar, cotton wool, non-woven gauze and sleek. Some products are provided by the hospital and others’ are purchased by patients. The types of wounds seen in FPRRH include pressure ulcers (PU), diabetic foot ulcers (DFU), surgical wounds (dehisced and evisceration), burns and maternity wounds. Many patients must travel long distances to attend the hospital and during their stay, have attendants who sleep on the floor and provide support, food, and routine care. This can create congestion, increase the risk of hospital acquired infections (HAIs), and make it harder to clean the clinical areas (Ackers et al, 2020).
Opportunities for exposure to frugal innovation in wound care
There is increasing interest in frugal innovation to address healthcare challenges in a low resource settings. In some cases, these innovations have been demonstrated to be preferable to more expensive alternatives (Tran and Ravaud, 2016). To aid the dissemination and adoption of potential frugal innovations, a digital compendium of frugal medical innovations was recently created by researchers from France (http://frugal-innovation-medicine.com/index.php). However, to date, this only contains one innovation related to wound care and refers to an article published in 1925 describing the use of ant mandibles as an alternative to sutures, a technique also used by ancient physicians (Majno, 1975). There has so far been little reported specifically on frugal innovation in wound care however, the authors believe that there are many opportunities for innovation within this field.
Frugal innovations are considered to fall into four discrete categories: lean tools and techniques, opportunistic solutions, contextualised adaptations, bottom-up innovations. Tran and Ravaud (2016) describe these as follows:
Lean tools and techniques, the simplification of existing technologies to reflect lower availability of resources. These technologies are not simply low-cost versions of more expensive technologies, but may be technologies with minimised functions to reduce costs. Examples of this in wound care may include, negative pressure wound therapy (NPWT) devices with limited functions to reduce manufacturing costs (Gopal and Solomon, 2016); the use of free range instead of bagged larvae; development of the World Alliance for Wound and Lymphoedema Care Wound Care Kit for less resourced countries, which contains sufficient material to produce up to 100 dressings (Vuagnat and Comte, 2016)
Opportunistic solutions, these are when contemporary technologies are used to address ‘old’ clinical problems. Examples include the use of patients’ smartphone cameras to document wound healing as an alternative to the acquisition and maintenance of expensive technologies by healthcare providers; video conferencing software to facilitate international consultation on clinical cases to obtain second opinions
Contextualised adaptations, this is the diversion of existing tools for different purposes. Examples include construction of NPWT from readily available hospital supplies (Vuagnat and Comte, 2016); the use of nappies as superabsorbent dressings; the use of sterilised banana leaves or boiled potato peels as dressings; use of green tea bags for wound odour management (Bolton, 2016); polyvinylidene food wraps as wound dressings and Papaya pulp for enzymatic debridement (Benskin, 2013).
The practice of contextualised adaptations in low- and middle-income countries (LMIC) may make health professionals in high income countries (HICs) concerned over the apparent lack of sterility or application of moist wound healing principles when using these methods. However, these practices are for conditions when contemporary dressings are unavailable due to costs and access to materials. For example the World Alliance for Wound and Lymphoedema Care (WAWLC) dressing kit was developed from a DELPHI consensus study of experts and is based upon quality wound care in an emergency situation or in a situation with limited resources in health centres or district hospitals. These guidelines make reference to using products that provide ‘judicious infection control practices’ (Vuagnat and Comte, 2016). The Joanna Briggs Institute WHAM Node Low Resource Setting section also provides useful insights about the properties of frugal wound care innovations and for balance, the evidence summaries provide practical recommendations for their readers for example there is no published evidence on the use of potato peel dressings in chronic wounds (Haesler et al, 2022).
Bottom-up innovations use simple technologies to improve outcomes. Examples include boiling or salination of water for use during wound cleansing or irrigation.
To support low-resource healthcare settings achieve optimal clinical outcomes it is necessary for further investigation of frugal innovations to be conducted (Benskin, 2013). Ideally, approaches already common in these settings should be investigated using robust methodologies to identify opportunities to maximise the efficiency and efficacy of care and measure the efficacy of the adaptations.
Virtual wound clinic: frugal management and innovation case studies
In HICs, evidence-based practice drives high-quality wound care (National Wound Care Strategy Programme, 2022), whereas in LMICs wound care practice is based on affordability and accessibility of products (Gupta et al, 2021). Despite these different approaches, the purpose of the virtual wound care clinics was to examine the global management of wounds and critically discuss practices to assist in reducing the impact wounds have on mortality, morbidity and healthcare resources. The clinics allowed the students to consider the impact frugal innovation can have on serving the needs of underserved populations which is to offer ‘low-cost and efficacious, new or adapted products (or services), mostly emerging from contexts of institutional voids and resource constraints, involving the creative use of existing resources’ (Sarkar and Mateus, 2022). The clinics also allowed staff in Uganda, to examine the current evidence base used to support care delivery, service provision and the role each member of the interprofessional team has to offer in the holistic management of patients with acute and chronic wounds. We will now describe four of the cases that were presented during the virtual wound clinics, showing comparisons in practices (Table 1) and highlighting the changes the midwives had instigated.
Case study 1: management of a patient with a dehisced abdomen and sepsis
A dehisced or burst abdomen is a serious complication of intra-abdominal surgery where abdominal muscles separate exposing the abdominal contents, carrying significant morbidity and mortality. Wound infection, coughing, malnutrition, emergency surgery and anaemia increase the risk of burst abdomen (Soni et al, 2015). There are no prevalence rates of burst abdomen in Uganda, but it is seen regularly in gynaecology in FPRRH. This case describes the care of a girl presenting with a burst abdomen.
A 17-year-old female presented with obstructed labour and proceeded to emergency caesarean section. She was discharged the following day, while her baby was admitted to neonatal intensive care. After three days she was readmitted with pain around the wound, febrile, hypotensive, and tachycardic. Her abdomen was distended and tender, with pus discharging from the wound. Vaginal examination showed foul smelling lochia rubra. She was started on antibiotics and her stitches were removed to open the caesarean section wound. During the next few days, she began spiking high fevers, and presented with a distended and tender abdomen, offensive, green discharge was oozing from the wound. A laparotomy was performed, and profuse pus and necrotic tissue were discovered within the peritoneal cavity. The uterus was also necrotic. Pus was drained, uterine debridement performed and repaired, and the abdomen closed. After a further three days she developed a burst abdomen with profuse pus and was rescheduled for a laparotomy. However, she then tested positive for the Covid-19 virus and the surgeons were unable to operate. Instead, she was monitored for deterioration and had daily wound dressings, using an aseptic non-touch technique (ANTT), daily irrigation with saline and the wound dressed with sterile dry gauze. After two weeks the wound had granulated, with a gaped rectus sheath and therefore abdominal wall closure was performed. She was discharged home soon after.
During the virtual wound care clinic students and staff were asked questions to stimulate bilateral learning regarding how they would describe the type of wound presented in this case and the underlying aetiology (burst abdomen versus surgical dehiscence), what the clinical signs of infection are in an acute wound (erythema, heat, malodour, purulent discharge, pain, oedema, delayed healing, loss of function), how the wound and patient should be managed (based on local resources and then comparisons globally) and closure of the wound versus closure of the rectus sheath and healing by secondary intention. Interestingly the clinical signs of infection led to discussion of the term erythema as both countries reported this as a clinical sign of infection at the wound bed. Pictures of the patient’s wound were then examined and those present were asked to describe what they saw. It was agreed that erythema was not visible, but instead differences in skin colour were noted between the periwound area and surrounding skin. This led to a discussion regarding the latest Best Practice Statement in the UK (Wounds UK, 2021) that examined skin tone bias in wound care. Those present also discussed the use of sterilised mosquito nets for abdominal wall repair, which is common practice in LMIC for hernia repairs (Tongaonkar et al, 2013). A recent clinical review by Skopec et al (2021) found that mosquito net mesh more closely resembles the biological and mechanical properties of the abdominal wall and, therefore, is more suitable for use in hernia mesh repair. This calls for a clinical trial to provide grade 1 evidence for its cost-effectiveness and efficiency of use in the UK.
Case study 2: management of a patient with an infected diabetic foot ulcer
Diabetes is a chronic, progressive condition with many complications. DFUs occur following poor glycaemic control, secondary to neuropathy and ischaemia (Yazdanpanah et al, 2018) and carry significant morbidity and mortality. A meta analysis found 14.2% of patients hospitalised for a DFU (or complication due to a DFU) died (Rigato et al, 2018). Prevalence of diabetes across Uganda may range from 1.4% to 9% (Mondo et al, 2013; Bahendeka et al, 2016), with rates as high as 16% in rural areas (Chiwanga et al, 2016). Most patients with diabetes have never been diagnosed (Rigato et al, 2018), but even with a known diagnosis there is suboptimal control in 42.8% of patients, with 31.2% having diabetic neuropathy (Kibirige et al, 2014).
A 50-year-old female diagnosed with type II diabetes (four months before admission), treated with metformin and glibenclamide, presented with a DFU. She had a two-week history of swelling of the right big toe and dorsum of the foot, associated with excessive urination, blurred vision, and numbness of the lower limbs. Her physiological observations were normal, but a random blood sugar was high at 20mmol/l. Her right foot and leg were swollen with oedema to the knee. The distal toe was darkened and dry. The dorsum of the foot appeared yellowish, covering an area of 10cm x8 cm with a sinus discharging pus. An incision was made across the DFU, allowing pus to drain. Necrotic and gangrenous tissue were removed, then cleaned using hydrogen peroxide. She was treated with IV antibiotics, and subcutaneous insulin for diabetic control. Her insulin was adjusted according to her blood glucose but remained high. She underwent daily dressings using ANTT. The wound was cleaned using diluted hydrogen peroxide. The remaining necrotic tissue was removed on the ward, then irrigated with sterile saline. It was packed with honey gauze and dressed with dry sterile gauze.
Debridement was repeated after five days as the wound continued to produce exudate. Pus was drained and the edges and base were thoroughly cleaned. The wound was dressed using sterile gauze soaked in iodine. The patient was discharged the following day on oral antibiotics and encouraged to seek dressing changes at her local health centre.
During this clinic those present were asked to examine how they would define what a DFU was, what the causative factors were for the presenting case, what assessment tools could be used to aid diagnosis and management including the dressing type and footwear. Significant discussions took place on the merits of hydrogen peroxide as a wound cleansing agent, as its use in practice in the UK has declined due to the toxic effects on healthy tissue and fibroblasts (Rueda-Fernández et al, 2022). This assisted the Commonwealth Fellows in challenging current practices within FPRRH as they tried to move to normal saline being the only option for the cleansing of wounds.
Case study 3: management of a child with a burn injury
Paediatric burn injuries are the third most frequent cause of injury and death globally in children (Chikwanha et al, 2013). Those injuries can be devastating especially in LMICs due to increased risk factors such as unattended children at home, crowding, and using the kitchen as a room to sleep; in addition to few trained burn specialists and burn centres available (Chalya et al, 2011).
Patients suffering from grease burns, such as cooking oil, are at higher risk of developing deep wounds due to the heat (higher boiling point) and thick, sticky and semi-fluid consistency (Klein et al, 2005). Grease burns have a much higher rate of requiring excision and grafting.
Minimal data indicates children constitute the highest proportion of the burn victims in Kampala (Nakitto and Lett, 2010). FPRRH is observed to have weekly admissions on the paediatric ward for accidental burns.
A three-year-old girl presented to the ward with burns to multiple body parts caused by accidently falling into hot cooking oil. On examination, approximately 20% total body surface area (TBSA) was affected with blisters and peeling skin involving trunk, full length of both upper limbs, and face. Initial observations did not indicate an infection and the child appeared in stable condition. The diagnosis was 20% mixed-thickness burns. The typical management plan for this condition included IV fluids, pre-emptive IV antibiotics and administrations of Tetanus toxoid. Pain was managed with rectal paracetamol. Within 24 hours, the patient had wound debridement under general anaesthetic. The wounds were cleaned with normal saline and silver sulfadiazine (SSD) was applied. Wounds were then dressed in Vaseline/petroleum gauze. Grafting was not performed as this was not available in this setting. The dressing was changed every four days until the wound improved, and no bleeding was noted. After 17 days, the patient was discharged on oral antibiotics for five days and continued with dressing changes at the nearest health centre.
Prompt intervention of paediatric burns caused by cooking oil is needed and while this patient presented the day after the injury, this is considered quick as commonly patients present days or weeks later. Surgery within 24 hours was efficient as frequent delays occur due to the lack of staff. Studies show that early intervention in burn management is vital due to the risk of developing septicaemia (Rowan et al, 2015). This case raises the question whether IV antibiotics throughout their admission was necessary (Stewart et al, 2015) creating an opportunity for more research.
Discussions during this virtual wound clinic centred around the use of SSD and Vaseline impregnated gauze. A systematic review and meta-analysis (Nimia et al, 2019) compared the effect of silver sulfadiazine (SSD) with other new dressings, with or without silver, on healing and infection prevention in burns. The authors concluded that ‘new dressings with and without silver show better results than SSD for wound healing, and burns treated with dressings without silver are less likely to become infected than burns with SSD. No differences between SSD and new silver materials were observed in relation to infection prevention’. While this assists in delivery of evidence-based practice in HICs, in LMICs many modern dressings are unavailable, and studies that evaluate the use of impregnated tulle gras on time to wound healing would be of clinical use (Sahin et al, 2019).
Case study 4: management of a patient with a pressure ulcer
PUs are areas of damaged skin and underlying tissue following constant, prolonged pressure causing cessation of oxygen and nutrition leading to tissue ischaemia (Bhattacharya and Mishra, 2015). A recent meta-analysis estimated the prevalence of PUs throughout Africa to be 11% (Anthony et al, 2021). Many factors increase the risk of PUs including hypertension, malnutrition, increasing age and immobility (Agan et al, 2018).
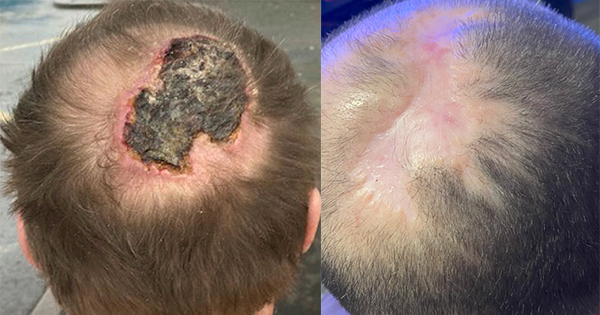
A 52-year-old female was admitted with extensive category 4 gluteal PU (European Pressure Ulcer Advisory Panel [EPUAP] et al, 2016) and other smaller wounds following four-months in bed, secondary to paraplegia of unknown cause. There was major skin and tissue loss which involved the muscle, bone and tendon (Zaidi and Sharma, 2021). There were signs of infection tracking surrounding the wound. On examination she appeared malnourished with bilateral lower limb oedema. She was hypertensive. Lower limbs had a power of 1/5, were hypertonic and without reflexes. She has no relevant past medical history. A culture and sensitivity swab isolated Escherichia coli, Acinobacter, Proteus mirabilis and Enterococcus spp. Her liver function, complete blood count and renal function tests were normal. She had a chest and lumbosacral x-rays, to investigate the cause of her paraplegia, the results of which were normal. Ultimately no cause was found. She required a blood transfusion on admission and was treated with antibiotics.
She underwent daily dressings using ANTT with normal saline and gauze. Sugar paste was applied making sure the cavities were filled then dry sterile gauze was applied followed by strapping.
Unfortunately, despite all efforts using a multidisciplinary team approach, this patient died of septic shock.
Virtual wound clinic discussions took place on the direct and indirect causes of PUs, categorisation of PUs, wound swabbing and reporting processes, the over prescription of antibiotics and the use of sugar paste. The therapeutic benefits of sugar for the management of wounds is noted to include a decrease in malodour by inhibiting bacterial growth, reduction in oedema, a change to the wound pH, thus increasing the bacteriostatic effect, stimulation of granulation tissue from local irritation, and growth of epithelial tissue (Kilic, 2001). However, a review of animal studies of sugar-based compounds on wound healing suggests topical applications are ‘safe and promote wound healing by their antibacterial, immunomodulatory and wound contraction effects’ (Oryan et al, 2019). The authors also noted that sugar-based compounds only have value on the initial stages of wound healing and certain types of wounds.
Discussion
Applying TIME in frugal wound management
Wound healing by activating the endogenous healing process along with effective therapeutic measures is an approach to wound bed preparation (Schultz et al, 2004). The TIME framework was initially proposed to have T–Tissue, I–Infection, M–Moisture and E–Epithelial migration. Epithelial migration was later modified to include E–Edges of wound. In 2019 this was updated to TIMERS to include R–Regeneration and S–Social Factors (Atkin et al, 2019) In FPRRH the original framework was recently adopted to enhance wound healing using innovative strategies to encourage normal wound healing with minimal interventions and locally available resources.
Tissue debridement of non-viable tissue is one of the first steps in wound bed preparation. Muhammad (2014) highlighted that clinical experience favoured a combination of surgical debridement followed by enzymatic debridement. Sharp or surgical debridement is carried out at the bedside or in the operating theatre in FPRRH.
Mechanical debridement, hydrogen peroxide and honey were used to debride the wound in the DFU case study. Hydrogen peroxide has fallen out of favour in many countries following concerns with local toxicity (Wilkins and Unverdorben, 2013). However, it remains common in LMIC settings where few alternative wound debriding agents are available. Hydrogen peroxide may improve healing of chronic wounds, but more research is required (Wilkins and Unverdorben, 2013). Clinically, honey is found to be beneficial for DFUs, which is supported by a review of multiple studies (Zhu et al, 2017). Honey reduces wound debridement time and bacterial clearance time (Wang et al, 2019). Honey is readily available in our low resource setting making it a sustainable wound management option.
Wound infections delay healing, therefore, are a key point of the TIME framework for wound bed preparation. Addressing local wound infection using appropriate dressings and topical antimicrobials can decrease bacterial load and promote healing.
In the management of the paediatric burn wounds sugar was used. Sugar has an osmotic effect reducing the moisture in the wound, which promotes granulation tissue formation and inhibits bacterial growth (Haynes and Callaghan, 2011). Sugar is beneficial in infected wounds (Biswas et al, 2010; Murandu et al, 2011) and is cheap and readily available. However, more recently sugar is no longer used at FPRRH because of concerns on sterility (people used ward sugar supplies for domestic purposes). However, if this issue is overcome, sugar could be used in wound management. In future, honey could be an effective alternative because it is easier to maintain sterility (Mphande et al, 2007).
Moisture balance is key in creating a moist wound environment for healing to occur. Petroleum jelly used in diaper rash decreases epidermal water loss (Alonso et al, 2013), and is known for its moisturising properties, when used for minor surgical procedures (Czarnowicki et al, 2016). Hanna and Giacopelli (1997) state the use of gauze impregnated with petroleum for surgical or traumatic wounds such as burns showed an increase in patient comfort and disruption to wound sites during dressing change. The secondary dressing of gauze provides some absorptive properties, although the risk of strikethrough is common with gauze dressings over more modern ones such as foams. Strikethrough breaches the dressing barrier, creating a pathway for bacteria to reach the wound bed. Furthermore, in the UK and America, the use of petroleum jelly is prescribed with caution in wounds and alternative moisturisers/dressings should be prescribed if a patient is on oxygen therapy or smokes. A small number of cases of burns to faces, scalp and hands have been reported in patients who have accidentally ignited themselves and/or their dressings (Bauters et al, 2016).
To assist with epithelial edge advancement surgical closure was an option for the patient with the burst abdomen. There is limited evidence for guidance, particularly in low-income settings on the management of burst abdomen. The European Hernia Society offers guidelines recommending the use of mesh but cannot comment on alternative methods due to lack of evidence, with management decided clinically due to heterogenicity of burst abdomen (López-Cano et al, 2018). Management options of primary closure with or without mesh, temporary closure, or conservative management with regular wound dressings with wet sterile gauze, or negative pressure dressings have been described (van Ramshorst et al, 2010). Conservative management may have increased morbidity with a longer healing time, therefore primary closure with mesh is often recommended (Jaiswal and Shekhar, 2018; Denys et al, 2021; Hermawan et al 2021). The surgeons at FPRRH chose primary closure of wounds without mesh, despite understanding the long term risks of herniation for the patient (Bosanquet et al, 2015). However, due to the Covid-19 pandemic this patient was managed conservatively. Dry gauze was used in this instance due to the level of exudate and pus, however wet gauze potentially with honey as an adjuvant could be used as described in the literature (Jaiswal and Shekhar, 2018).
Reflections on frugal management and innovation on future practice
Frugal management and innovation have been central to the project, two wound dressing companies attended a pilot virtual clinic sparking an interest in the development of a wound dressing for LMICs (Fit4Purpose®). With support of a UK microbiology volunteer, K4C has developed a ‘honey gauze’ dressing using locally made medical grade honey, reducing reliance on antibiotics and antiseptics on the ward. An improvement in rates of sepsis and a reduction in sepsis deaths have been observed in the findings of an action research intervention (Ackers et al, 2020). Discussions with Joint Medical Stores, the primary supplier of medical supplies in Uganda, to enable distribution for honey gauze nationwide is now underway.
The volunteers and University of Salford students identified that they learnt about frugal practice, while gaining a deeper understanding of the scarcity of essential items. This gives a renewed appreciation of the National Health Service (NHS) and its resources. The evidence base for many aspects of frugal practice is rooted in low-resource settings, and knowledge sharing through virtual clinics provides understanding of its application, including use in the NHS. For example, the workshops highlighted evidence-based practice such as the use of water for wound cleansing and honey for the antimicrobial, antioxidant, and anti-inflammatory properties.
The clinics have also impacted the development and/or revision of guidelines both in the UK and Uganda and allowed the examination of skin tone bias and signs and symptoms of wound infection in patients with dark skin tones. Reflecting on our experiences within the virtual wound clinics, it is apparent that further visual learning materials in the form of wound images showing clinical signs related to colour are needed to support learning in this area. The Wounds UK (2021) best practice document on skin tone bias does not provide images like this across the skin tone spectrum currently. This is important to ensure timely identification of common wound complications including infection and vascular disease. The international relevance of health education curricula and virtual learning alliances such as this, play a role in dismantling Eurocentric healthcare curricula (Liyanage, 2021), increasing accessibility, diversity, and inclusivity, and creating a global workforce for the NHS and beyond.
Conclusion
The challenge of delivering wound care in low resource settings directly impacts patient outcomes, however opportunities can arise from frugal innovation and a multidisciplinary approach to wound care delivery. The creation of virtual wound care clinics across two global communities provided learning for professional and academic development of students on a postgraduate tissue viability module in Salford. In also created links between the university and clinicians in Uganda to develop delivery of evidence-based wound management using minimal resources. Unexpected learning included the development of a honey wound dressing, revision of evidence-based guidelines, and examination of skin tone bias in the signs and symptoms of wound infection in patients with dark skin tones.