Advances in medical treatments and equipment are increasing life expectancy (Raleigh, 2022). Correspondingly, the population in England and Wales has continued to age, and in 2021, over 11 million people (18.6% of the total population) were aged 65 years old or older (Office for National Statistics, 2022).
As people live longer, the healthcare challenges they face increases. These include pressure ulcers, which are responsible for 5% of all wounds in the UK and 7% of the total NHS spend on wound care (Guest et al, 2020). The economic cost of pressure ulcers is estimated at £3.8 million per day (NHS Improvement, 2018). The human cost and suffering associated with pressure ulcers and their treatment is also profound; Lyder et al (2012) reported that patients who developed a hospital-acquired pressure ulcer were more likely to die during their hospital stay, generally spent longer in hospital, and were more likely to be readmitted within 30 days of discharge.
Patient comfort and rest are required for improved well-being and recovery (Langemo et al, 2017). Unfortunately, achieving these in hospital can be extremely difficult. This is due to intrinsic factors, such as discomfort, pain and anxiety, and extrinsic factors, including excessive noise and frequent clinical interventions. These factors negatively affect physical and psychological status, which can lead to deconditioning, impaired recovery and increased length of stay (Morse and Bender, 2019). Early mobilisation, which has been shown to be associated with improved outcomes (Stephenson, 2018) can also be affected. The choice of mattress can have a positive or negative impact on many factors which contribute towards holistic care (Caggiari et al, 2021).
Medstrom has been supplying and developing therapeutic mattresses for many years. This includes the Dolphin Therapy fluid simulation support surface that was first introduced in the UK in 2012. To date, fluid immersion/air fluidised is one of the only viable ‘step up’ options from a dynamic air mattress (Nursing Times, 2022). Data collected for over 3000 highly complex patients nursed on the Dolphin Therapy fluid immersion surface to either prevent or treat skin damage supports its efficacy (Medstrom, 2023). It has demonstrated consistent and outstanding outcomes for pressure area care and other key objectives in regard to extremely complex and difficult-to-manage patients.
Dynamic air mattress technology has not changed much in the last 20 years. New variants of the same dynamic air mattress technologies have been introduced, but these essentially perform in similar ways to their predecessors, with no real difference in patient outcomes. Recognising the need for a new solution to meet the demands of an ageing population, and in response to customer feedback, the Aria air mattress range was developed (Figure 1). Its novel air immersion technology is designed to fulfil the following objectives:
- Provide a better alternative to old mattress technology to meet the needs of an ageing population who require a high specification mattress for treatment or prevention of skin damage, but do not require a fluid immersion or air fluidised support surface.
- Allow seamless ‘stepping down’ from or ‘stepping up’ to a fluid immersion or air fluidised support surface.
- Offer reactive and active therapies as defined by the European Pressure Ulcer Advisory Panel (EPUAP, 2016), giving clinicians a choice of therapy modes to drive patient comfort and adherence to care
- Improve the patient and caregiver experience through the provision of a therapeutic air mattress.
To help achieve these objectives, the features incorporated into the Aria mattress range design include:
Dual modality, offering two therapy modes:
- Reactive: Constant immersion, providing continuous low pressure.
- Active: Gradient immersion (Box 1), providing subtle and cyclical pressure changes within the mattress cells.
Both modes respond to the patient’s weight and position on the mattress, and adjust each time the patient moves.
A third mode (Max Inflate) fills the cells to their maximum capacity for easier mobilisation to and from the bed. Operated by a single button, the Max Inflate mode defaults back to therapy after 20 minutes. Key features of Aria PRO include:
- Quiet control unit operation, emitting approximately half the noise of traditional dynamic control units (Medstrom, data on file)
- Cubed cells increase contact area for improved immersion and easier mobilisation compared to traditional circular cells (Figure 2).
Aria PRO has several additional features that help when nursing higher acuity patients, including:
- Deeper cells for increased immersion.
- Bridging cells which can replace standard cells for heel off-loading (Figure 3).
There are several mattresses in the Aria range, but this case series focuses on Aria and Aria PRO, which were first used in the UK at the end of 2020. As completely new products with novel technologies, it was important to gather evidence about their clinical efficacy and practicalities of their use. As a result, a series of 21 case studies was compiled. Pressure area care, patient experience, comfort, adherence to care and early mobilisation were explored, and this paper reports on and interprets the results.
Method
From July 2021 to March 2023, patients’ journeys were documented by Medstrom’s team of Clinical Advisors, who were already working closely with healthcare professionals and patients within NHS Trusts. Over 25 Clinical Advisors were involved in the study and data collection sheets were used to document the patients’ journeys. These forms collected information on the patient’s background, past medical history, skin integrity on admission and at discharge, treatment objectives and mode used (constant or gradient). Staff were asked to comment on any benefits they noticed, including product weight, ease of use, transport mode, efficacy, noise and level of immersion compared with other surfaces. Patients were asked to comment on their comfort and wellbeing while nursed on Aria or Aria PRO mattresses in contrast with other support surfaces. When the study commenced, all of the patients had been nursed, or were still being nursed, on an Aria or Aria PRO mattress. The patients’ details were anonymised before they were sent to Medstrom’s clinical research team for interpretation.
Results
Case studies were obtained for a total of 21 patients across 11 different sites (nine hospitals, one hospice and one patient’s home).
Patient Demographic
Of the 21 patients, 13 were female and 8 were male. The age of the patients was between 31 and 92, and the average age was 68 years.
All the patients had acute conditions at the time of Aria and Aria PRO placement, as shown in Figure 4. The most common chronic conditions that the patients presented with were ischaemic heart disease, heart arrhythmias, diabetes mellitus, dementia, chronic kidney disease, hypertension, cerebrovascular accident (CVA), chronic obstructive pulmonary disease (COPD) and spinal injury.
Pressure area care outcomes
Patient Risk Scores
Patients were categorised using several scoring systems that varied between hospitals and care settings. Risk score categories are shown inFigure 5. A total of 18 patients (86%) were classed as high or very high risk.
Prevention versus Treatment of Skin Damage
To interpret the skin integrity outcomes, patients were classified into two groups:
- Prevention: Patients without existing skin damage
- Treatment: Patients with existing skin damage.
Prevention Group
Following local protocol according to risk, ten patients out of 21 were placed on Aria or Aria PRO for prevention purposes. All were nursed using constant immersion and no patients developed skin damage.
At the time of data collection, one patient had spent 177 days bedbound in intensive care on an Aria PRO mattress. Her skin remained intact with no visible damage, and she felt much more comfortable when placed on an Aria PRO mattress than the traditional dynamic mattress she used previously.
Treatment Patients
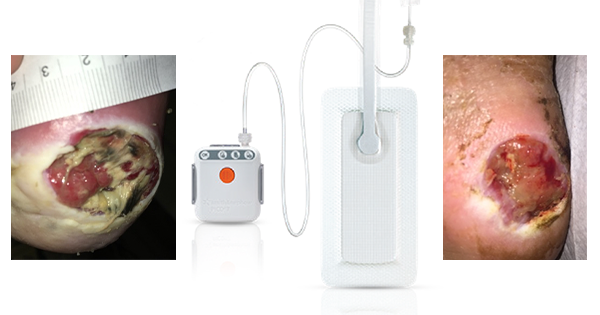
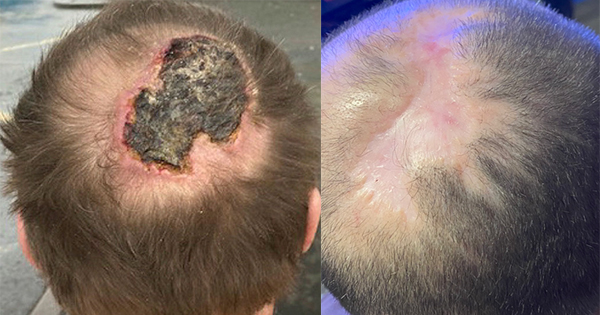
Eleven patients out of 21 were placed on Aria or Aria PRO for treatment purposes. Nine were nursed using constant immersion and two using gradient immersion. No clinical evidence currently exists to suggest that either type of therapy is better than the other (McInnes et al, 2015). In the present study, type of therapy varied between settings and was based on patient preference (e.g. comfort) with input from clinicians. There were 21 areas of skin damage recorded in total, with some patients having two or more damaged areas. Damage recorded included Category 1, 2, 3, 4 and unstageable pressure ulcers, deep tissue injury (DTI), moisture associated skin damage (MASD) and blistering (Figure 6A–B).
Of these 21 skin damage areas, the outcomes at the time of data collection were as follows:
- Healed: 7
- Improved: 13
- Remained static: 1
- Deteriorated: 0
During the study period, one patient, in the treatment group whose skin damage remained static, was ‘stepped up’ to Dolphin Therapy from Aria PRO due to general deterioration in their clinical condition and two were ‘stepped down’ from Dolphin Therapy to Aria PRO due to an improvement in their skin damage and clinical condition. After being ‘stepped down’ to Aria PRO, no skin deterioration was reported.
Additonal outcomes
Improved Patient Experience
Other objectives for swapping to Aria or Aria PRO from the previous surface that the patient was using included improved comfort, sleep, pain management, adherence to care, reduced turning frequency and early mobilisation.
For the majority of patients where these objectives were set, they were met. Where they were not, reasons included:
- Patient deteriorated
- Patient was confused and agitated
- Patient was non-compliant with nursing interventions.
Staff Feedback
Quotes from staff and general feedback was collected via data collection forms. Overall feedback from staff about Aria and Aria PRO was extremely positive and included the following:
- ‘The mattress is much lighter than previous ones, so one person can now set it up instead of two’
- ‘Patients who can’t tolerate the cell movement of older mattresses are more comfortable on Aria or Aria PRO’
- ‘The firm cell mode facilitates patient mobilisation’
- ‘The quiet operation of the control unit is helping patients to rest better’
- ‘Both mattresses are easy to use’.
Patient Quotes
Feedback from patients about Aria and Aria PRO was also positive and included:
- ‘The mattress is very comfortable. I’m sleeping better because it’s lessened the pain in my legs’.
- ‘I feel like the mattress is part of me and would like to go home with one’.
- ‘I can stand more easily from this mattress’.
Two patient journeys have been summarised.
Patient 1
A 70-year-old lady was admitted to hospital with urosepsis and hypovolaemic shock. She had a Category 3 pressure ulcer on her sacrum and a DTI on her heel, and both were acquired in the community.
On admission, the patient was placed on a traditional alternating pressure mattress; however, the Category 3 pressure ulcer deteriorated to Category 4 and was causing severe pain. She was transferred to a Dolphin Therapy fluid simulation support surface to help with pressure area care and pain management due to her complexities.
After 4 weeks, the patient’s condition had improved, and she was ready to start mobilising more. The Category 4 pressure ulcer had begun to heal, and the DTI was improving. She was ‘stepped down’ to Aria PRO with the constant immersion therapy mode selected.
The patient found Aria PRO comfortable and preferred it to the alternating pressure mattress that she had been on prior to Dolphin Therapy. The transition from Dolphin Therapy to Aria PRO was smooth and continued to provide comfort, aiding rest and recuperation. The Max Inflate mode helped to facilitate mobilisation and her mobility improved as a result.
At the time of data collection, the patient was still in hospital but was able to walk with a frame, which she had done prior to becoming unwell at home. The Category 4 pressure ulcer was smaller in size and improving, the DTI had healed and she had no new areas of skin damage.
Patient 2
A 74-year-old gentleman was admitted to hospital with aspiration pneumonia and resolving delirium.
He had no visible skin damage and was nursed on an Aria mattress from admission using the constant immersion therapy mode. Aria was selected because the patient was at high risk of developing pressure damage, and staff felt he would not tolerate the movement of a traditional alternating dynamic mattress due to his confused state.
As he was frail and initially bedbound, staff used the Max Inflate function to facilitate two-hourly repositioning.
After 2 weeks, the patient had improved physically and was a lot less confused. He started mobilising from the bed with assistance and a walking frame. The staff commented that the Max Inflate function facilitated this as it provided stability and a smoother transfer.
The patient was discharged home 4 weeks after admission, and on discharge, he could stand with the assistance of one person and was able to mobilise using a walking frame. His skin remained intact with no visible damage throughout his entire stay in hospital.
Overall, the patient found the Aria mattress comfortable. Staff fed back that the constant immersion therapy not only protected his skin, but also helped improve adherence to care due to the comfort of the mattress and the fact that the cells were not actively moving. They also felt that the ability to fully inflate the cells helped with earlier mobilisation and ultimately the patient’s recovery.
Discussion
The outcomes observed in the case studies and the feedback reported from both patients and staff were positive. However, the study was limited in size and more data is required to further validate and build on its findings. Due to changing needs and changing risk, some patients transitioned from fluid immersion to air immersion technologies and vice versa. This demonstrates the importance of matching support surface choice to the individual on an ongoing basis, which is dependent on clinical status and patient objectives. It supports the need for a ‘right patient, right product, right time’ ethos to effectively achieve improved patient outcomes, as opposed to a ‘one size fits all’ mindset.
Objectives for the Aria and Aria PRO mattresses appear to have been achieved for most of the patients in this study. Both mattresses provided a suitable solution for patients who required an enhanced level of support, but did not need as high a specification as fluid immersion or air fluidised. ‘Stepping up’ and ‘stepping down’ from Dolphin Therapy was achieved successfully, and both constant and gradient immersion therapy were used with good effect. The overall outcomes for pressure area care were excellent; none of the patients in the prevention group developed skin damage at the time of data collection, and only one patient’s condition remained static in the treatment group.
Aria and Aria PRO also helped to improve the overall patient experience. Positive outcomes were gathered from the data collection forms, including improved comfort and rest. This contributed to increased adherence to care for some patients. Dual modality (constant or gradient immersion) was also noted as a contributing factor to adherence to care, as it provided a choice of therapies which could be matched to a patient’s preference or tolerance level. Of the patients that had capacity, none fed back that the mattress was uncomfortable, regardless of mode used. A key advantage of the Aria and Aria PRO mattresses is that it is possible to change the mode by pressing a single button to switch between gradient immersion, constant immersion and firm (Max Inflate) instantaneously. It was documented that the Max Inflate function helped to facilitate mobilisation in 8 patients. Ten patients out of the 21 were bed bound or hoist transferred. The remaining 3 patients may have used Max Inflate for mobilisation, but this wasn’t documented. All these factors can contribute to faster recovery and improved outcomes.
From the staff perspective, manual handling risks were reduced due to the lighter weight of the mattress, easier patient repositioning and simpler patient mobilisation. According to feedback collected via the data collection sheets, the improved patient satisfaction due to positive outcomes was also of benefit to staff. Some staff commented that ‘both mattresses are easy to use’, implying that the ease of use and similarities in the controls for both mattresses helped to ensure correct use.
A reduction in pressure ulcers decreases the documentation and dressing time required for their management. Overall, time can be freed up to be able to carry out other tasks.
The high-level objectives of the National Wound Care Strategy Programme (2023) are to improve patient care, reduce patient suffering, improve healing rates, prevent wounds occurring and reoccurring and increase productivity of staff. Aria and Aria PRO were able to help achieve some or all of these objectives for the majority of patients in this study.
CONCLUSION
The outcomes from these case studies are encouraging; however, more research is required to build on the initial clinical evidence. For this reason, data collection is ongoing, and results will be updated and published when new milestones are reached.