This meeting report is based on a ‘Made Easy’ workshop delivered at the Wounds UK Annual Conference in Harrogate in November 2025. The session was supported by an educational grant from Coloplast Ltd.
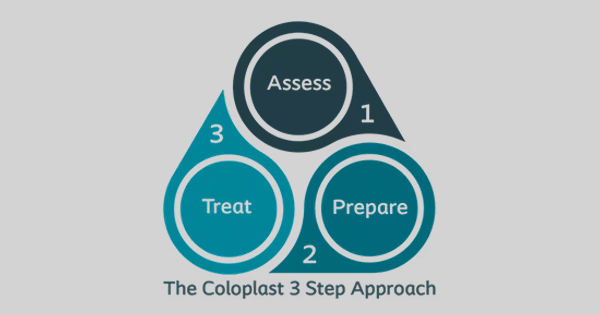
The workshop was chaired by expert tissue viability clinicians with extensive NHS experience and explored a simplified, standardised approach to wound healing. The 3 Step Approach by Coloplast: Assess, Prepare and Treat, was used as the central framework to guide discussion and clinical decision-making. Through interactive discussion and a real-life patient example drawn from clinical practice, the session aimed to provide clinicians with a practical tool to enhance wound care in everyday clinical settings. This approach was aligned with evidence demonstrating improvements in wound healing outcomes, clinician confidence and consistency of care when a simplified, standardised framework is applied (Atkinson, Orig and Vernon, 2024).
Wound care can often feel complex due to the wide range of available products and the diverse needs of patients with chronic or hard-to-heal wounds. While the session focussed on these more challenging cases, it also highlighted that the same standardised framework can be applied to simpler wounds, promoting increased clinician confidence and consistency in wound management.
The learning objectives of the workshop were to:
- Understand the principles underpinning The 3 Step Approach by Coloplast (Assess, Prepare and Treat)
- Strengthen skills in holistic wound and patient assessment
- Recognise the importance of effective wound preparation in removing barriers to healing
- Apply a standardised decision-making framework to support appropriate product selection
- Relate these principles to real-world practice through a patient example.
Background: Challenges in chronic wound management
Chronic wounds pose a significant challenge to healthcare systems, affecting patient quality of life, increasing the risk of infection and contributing to the burden on clinical services (Guest et al, 2020). The multifactorial nature of wound chronicity such as comorbidities, reduced perfusion, the presence of biofilm and increased risk of wound infection, excessive exudate and patient-related factors makes healing complex and unpredictable (Murray, West and McGuiness, 2018). Organisational and educational factors, including variation in practice and resource limitations may further contribute to delayed healing (Propper, 2024). In this context, there is increasing recognition that improving outcomes depends less on the use of numerous products and more on the reliable application of fundamental principles, underpinned by regular and systematic assessment.
Chronic wounds are often described as “stalled”, meaning they fail to progress through the normal phases of healing due to underlying barriers (Widgerow, 2012). These barriers include the presence of non-viable tissue or slough, poor moisture balance, bioburden, unmanaged exudate and deterioration of the wound edge or surrounding skin (Woulgan, 2016). If these barriers are not identified and addressed through standardised assessment and preparation, progression to healing is unlikely. Integrating consistent assessment and ongoing wound preparation into routine care can support earlier identification of these barriers and help re-establish progress towards healing.
Frameworks such as the Triangle of Wound Assessment support clinicians to systematically evaluate the wound bed, wound edge and periwound skin (Dowsett and von Hallern, 2017). This standardisation improves consistency, helps identify priority care needs and provides a clear rationale for selecting appropriate treatment. Such standardised assessment aligns with the first step of The 3 Step Approach by Coloplast (Assess).
International guidance documents highlight the need for thorough wound preparation, recognising that effective wound management extends beyond the wound bed alone to include the wound edge and surrounding periwound skin, alongside optimal exudate control and vigilance for signs of biofilm and infection. This broader, holistic approach is reflected in the Alprep® Pad best practice recommendations (Barrett et al, 2022). These principles underpin The 3 Step Approach by Coloplast, which focusses on assessing the wound and patient, preparing the wound by removing the barriers to healing and treating with an appropriate dressing selection.
By focussing on the fundamentals, cleansing and preparing the wound (including debridement), managing moisture and exudate, and supporting ongoing healing, a standard framework can be applied to a range of wound types (NHS Worcestershire Acute Hospitals, 2025). This standardisation is particularly valuable in busy community and acute care settings where clinicians may encounter a wide spectrum of wounds and can empower clinicians with a reproducible, easy-to-apply approach that integrates seamlessly into everyday clinical practice (Samarasinghe, Millar and Exworthy, 2024).
The 3 Step Approach by Coloplast: Simplifying wound healing
The 3 Step Approach by Coloplast provides clinicians with a simplified framework for wound healing. It is supported by a simplified portfolio of Coloplast wound care products, designed to help clinicians apply each stage of the framework in line with best practice recommendations and to support clinical decision-making. The approach consists of three core steps:
- Assess
- Prepare
- Treat (Atkinson et al, 2024).
This structure helps ensure that essential elements of wound care, particularly wound preparation, are not overlooked in busy clinical environments (Kamolz and Wild, 2013).
Step 1: Assess
Carry out a holistic patient and wound assessment to define clear preparation and treatment objectives. Assessment extends beyond the wound itself to include patient-related factors, as well as educational and organisational considerations that may influence healing and continuity of care. Standardised tools such as the Triangle of Wound Assessment support a holistic, systematic assessment of both the patient and the wound. This approach focusses on the wound bed, wound edge and periwound skin, to inform management goals and identify barriers to healing such as non-viable tissue, slough or suspected biofilm (Dowsett and von Hallern, 2017). The Triangle of Wound Assessment provides a standardised method for assessing these three components of the wound and supports the Assess step of The 3 Step Approach by Coloplast. Its use at initial assessment and during regular reassessment helps identify early signs of change, such as increased exudate, maceration, inflammation or changes to the wound margin, which may otherwise be overlooked (Dowsett, Swanson and Karlsmark, 2019). This comprehensive assessment guides appropriate wound preparation and dressing selection.
Step 2: Prepare
Within The 3 Step Approach by Coloplast, wound preparation focusses on removing barriers to healing and creating an optimal wound environment. This includes cleansing and debridement to remove slough, debris and biofilm. Wound preparation focusses on what is removed from the wound rather than what is applied to it. Regular and effective preparation improves visibility of the wound bed, supports accurate reassessment and reduces the risk of delayed healing or infection. As part of this step, the Alprep® Pad by Coloplast is used to support gentle, effective mechanical cleansing and debridement (Atkinson, Orig and Vernon, 2024).
Step 3: Treat
Treatment is guided by findings from the assessment and should address the underlying aetiology while supporting ongoing healing. Dressings should manage exudate, maintain moisture balance and protect the wound edge and periwound skin. Selecting dressings that conform closely to the wound bed helps minimise dead space, commonly referred to as the gap between the wound bed and the dressing. Effective management of this gap supports exudate control and reduces the risk of infection and delayed healing (Greco et al, 2020). Consensus guidance recognises that the majority of chronic wounds are relatively shallow, with evidence indicating that nearly 80% are less than 2cm in depth (Braunwarth et al, 2017). In line with this, international consensus reports that 83% of wound experts agree that for wounds up to 2cm deep, the optimal dressing choice is one that conforms closely to the wound bed (Keast et al, 2020). Dressings with 3DFit Technology** such as Biatain® Silicone and Biatain® Silicone Ag, are examples of products that support this approach through different stages of healing.
Case study: Applying The 3 Step Approach by Coloplast in practice
A key element of the workshop was a real-life patient example drawn from clinical practice, used to demonstrate how The 3 Step Approach by Coloplast can be applied to support progress in patients with chronic wounds.
Patient background
The patient was a 65-year-old woman with a medical history of hypertension, hyperlipidaemia, coronary artery atheroma and hyperuricaemia. Her medications included ramipril, amlodipine, bisoprolol, allopurinol and atorvastatin. She had successfully undergone a triple coronary artery bypass graft but suffered postoperative wound complications from the leg donor site.
At presentation, the postoperative wound on her right leg displayed delayed healing, with devitalised tissue present in the wound bed (combination of wet and dry slough), moderate exudate and oedema to the periwound skin. The wound had failed to progress despite previous interventions. Use of The 3 Step Approach by Coloplast enabled clinicians to reassess the wound and identify key barriers to healing.
Assess
A holistic assessment of the patient including full lower limb assessment and the wound was conducted, supported by the Triangle of Wound Assessment. This standardised assessment helped identify non-viable tissue, the condition of the wound edge, periwound skin issues and the need for more consistent wound preparation and a simplified treatment regime. Patient-related factors, including comorbidities, concordance and wound-related factors such as infection and pain, were considered as part of the assessment process.
Prepare
Wound preparation focussed on cleansing and debridement to remove slough and suspected biofilm to reduce wound bioburden and improve the visibility of the wound bed for accurate assessment. Regular preparation was essential to remove ongoing barriers to healing and support an effective dressing regime. Alprep® Pad with saline were used to support gentle, mechanical cleansing and debridement in line with the patient’s tolerance.
Treat
A simplified dressing regime was guided by assessment findings and aimed to manage exudate, maintain moisture balance and protect the wound edge and periwound skin. Dressings with 3DFit Technology, including Biatain® Silicone, supported this need by conforming to the wound bed up to 2cm in depth** helping to reduce exudate pooling and leakage, and maceration of the surrounding skin.
Reduced compression was used, in line with patient choice, to support venous return and manage lower limb oedema throughout treatment and ongoing care post-healing, despite a normal ankle brachial pressure index (ABPI).
Despite best efforts, wound infections may occur, requiring clinicians to manage symptoms and contributing factors. When signs and symptoms of localised infection were noted, such as erythema, increased pain and wound exudate, a simple switch to an antimicrobial dressing of Biatain® Silicone Ag with 3DFit Technology was selected and was easily adopted and accepted by the patient.
The treatment changed to Biatain® Silicone after two weeks when symptoms resolved.
The consistent use of Biatain® range dressings increased patient acceptance and concordance with the treatment regime, making supported self-management easy to adopt once the wound became stable. This greatly aided patient empowerment and improved quality of life with fewer clinic visits.
Product focus in practice
Product selection should be discussed within the context of clinical assessment and wound need rather than as a starting point for care. Within this framework, a simplified portfolio of Coloplast wound care products are selected to support The 3 Step Approach by Coloplast and should only be considered after thorough assessment.
Alprep® Pad
Alprep® Pad is a single-use cleansing and debridement pad designed to support gentle* mechanical removal of slough, debris, biofilm and non-viable tissue. Alprep® Pad is a tool that supports the “Prepare” step of The 3 Step Approach by Coloplast by helping remove barriers to healing. The two-sided design of the Alprep® Pad facilitates both cleansing and debridement of the wound bed, edges, and periwound skin, supporting regular and effective wound preparation (Barrett et al, 2023).
Biatain® Silicone
Biatain® Silicone is an absorbent silicone foam dressing designed to reduce exudate pooling and protect the wound edge and periwound skin from maceration. Effective exudate management is a key component of promoting optimal wound healing, and managing dead space (the gap) is recognised as an important factor in supporting this process (Keast et al, 2020). Close contact with the wound bed helps reduce dead space (the gap) and support effective exudate management.
Biatain® Silicone, incorporating 3DFit Technology, supports this need by conforming up to 2cm in depth**, helping to minimise gap formation. This reduces exudate pooling and helps reduce leakage and maceration of the surrounding skin (Colboc et al, 2024).
Building clinical confidence: Practical tips for everyday wound care
The workshop concluded by reinforcing the value of a simplified, standardised approach to wound healing that can be used by all healthcare professionals treating wounds and applied consistently across different care settings. By repeatedly returning to The 3 Step Approach by Coloplast: Assess, Prepare and Treat, the session demonstrated how a simple framework can support confident clinical decision-making and reduce variation in practice.
Effective wound care does not require multiple tools or complex algorithms, but rather consistent application of core principles within a simplified, standardised framework that supports both clinicians and patients. This approach emphasises embedding standardised assessment, ongoing wound preparation and appropriate treatment selection into routine practice to provide a practical pathway of care, support clinical decision-making, and enable progress towards healing.